Mood & Cognitive Function
Neurocognitive stability emerges from coordinated hormonal signaling, inflammatory balance, nutrient status, and stress modulation.
Systemic impact
Neurocognitive function reflects coordinated interaction between endocrine signaling, inflammatory tone, nutrient availability, and stress-axis modulation. Disruption in these interconnected systems rarely presents as isolated psychological phenomena.
It may manifest as:
-
Reduced cognitive clarity or slowed information processing
-
Irritability or affective variability
-
Sustained mental fatigue despite adequate rest
-
Diminished motivation or executive drive
These patterns often correspond to shifts in metabolic support, micronutrient-dependent neurotransmitter pathways, or stress-related regulatory signaling. Within this context, BodyMap provides structured orientation to support clinical interpretation and further assessment when indicated.
Regulatory drivers
Gut–brain axis
-
Microbial metabolites contribute to neurotransmitter modulation, including serotonin and GABA pathways
-
Dysbiosis may alter inflammatory signaling and neurochemical balance
-
Food reactivity can amplify systemic inflammatory tone influencing cognitive and affective stability
B-vitamins & micronutrients
-
B-vitamins (B6, B9, B12) act as co-factors in monoamine neurotransmitter synthesis
-
Magnesium contributes to neuromuscular relaxation and stress adaptation
-
Iron and iodine support oxygen delivery and thyroid-mediated cognitive regulation
Omega balance
-
Omega-3 fatty acids (EPA/DHA) support neuronal membrane integrity and anti-inflammatory modulation
-
Excess omega-6 relative to omega-3 may promote neuroinflammatory signaling
Circadian & sleep regulation
-
Sleep architecture influences synaptic consolidation, attention stability, and emotional processing
-
Melatonin–cortisol dynamics modulate daily neurocognitive performance
Stress & inflammatory load
-
Chronic stress may alter monoamine availability through sustained cortisol signaling
-
Inflammatory mediators can influence blood–brain barrier permeability and cognitive clarity
Professional Integration
Laboratory testing provides point-in-time biochemical measurements. However, isolated markers do not always reflect longitudinal regulatory patterns influencing neurocognitive stability.
BodyMap introduces a pattern-based, integrative layer by identifying functional trends reflected in hair-derived data.
Within the Mood & Cognitive Function domain, the report may surface:
-
Micronutrient distribution patterns relevant to monoamine neurotransmitter pathways
-
Fatty acid balance influencing neuronal membrane integrity and inflammatory modulation
-
Stress- and inflammation-linked regulatory signals associated with cognitive variability
-
Gut-related patterns potentially affecting the gut–brain interface
-
Endocrine indicators (thyroid, cortisol dynamics) influencing attentional and motivational stability
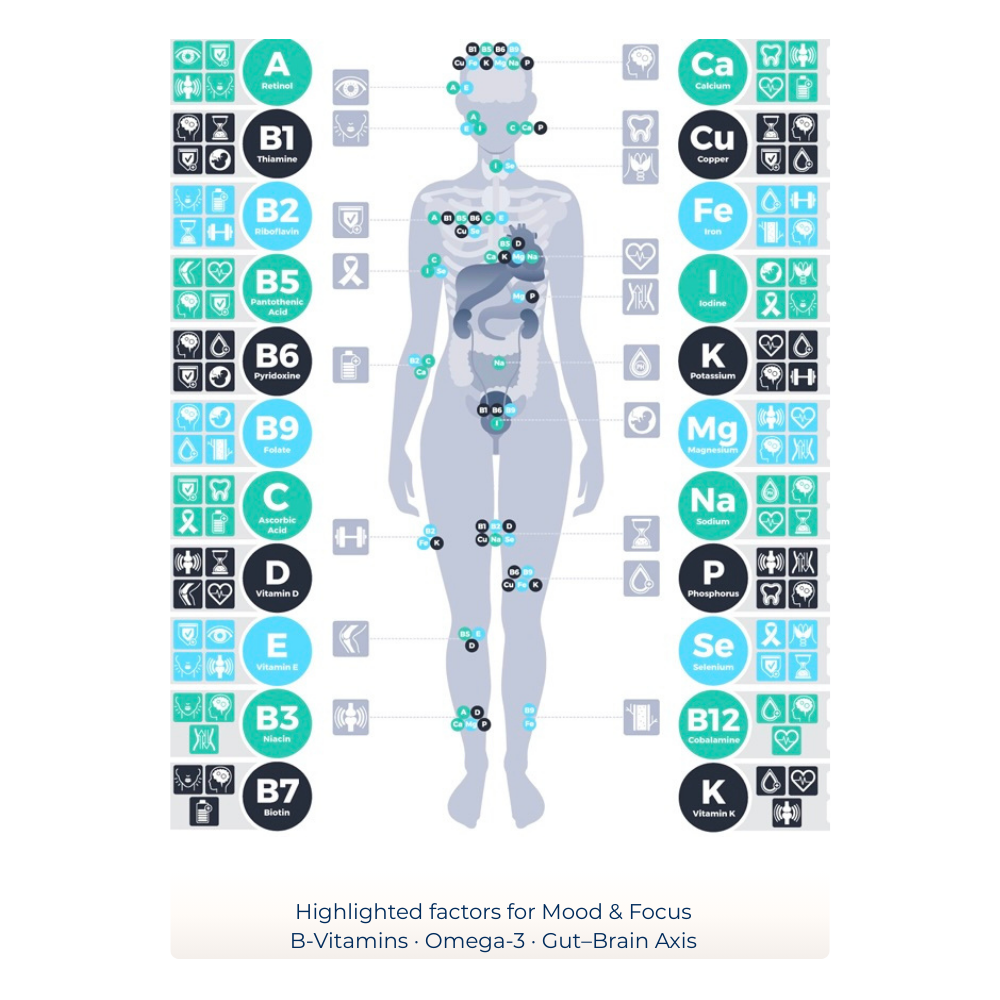
These findings are not diagnostic outputs. They function as orientation markers that may support structured interpretation and guide further clinical or laboratory assessment when indicated.
Report outputs
BodyMap translates identified patterns into structured orientation layers.
The report may include:
-
Nutritional axes relevant to fatty acid balance and micronutrient-dependent neurotransmitter pathways
-
Prioritization of micronutrient distribution patterns associated with cognitive and affective regulation
-
Lifestyle modulation domains influencing sleep architecture, stress-axis stability, and circadian coherence
-
Sequenced intervention priorities to support structured, non-fragmented implementation
This framework supports integrative decision-making rather than isolated or reactive adjustments.
FAQ
Here are some of the most common questions about mood, cognitive function and how BodyMap can help.
In which situations can BodyMap support mood or cognitive performance concerns?
BodyMap may support cases where concentration instability, mental fatigue, mood fluctuation, or cognitive resilience decline persist despite conventional lifestyle strategies.
It structures systemic regulatory signals that may influence cognitive clarity beyond isolated psychological factors.
How does BodyMap approach the gut–brain interaction?
The gut–brain axis is increasingly discussed in research and clinical contexts as a bidirectional regulatory pathway linking digestion, immune signaling, stress response, and cognitive function.
BodyMap does not claim to measure neurotransmitters or neural activity.
It structures functional signals related to inflammatory tone, micronutrient availability, stress modulation, and gut-related patterns that may influence cognitive clarity and mood stability.
This supports professionals in exploring systemic contributors without reducing cognitive concerns to a single mechanism.
Where does BodyMap fit in the evaluation of mood or cognitive instability?
BodyMap is positioned as a regulatory orientation tool.
It may help professionals explore whether nutrient signaling, stress modulation, inflammatory tone, or gut-related regulation could be contributing to cognitive fatigue or mood variability before escalating toward more specialized pathways.
It supports a structured inside–outside evaluation rather than replacing psychological or behavioral approaches.
What practical value does BodyMap add in mental clarity or performance environments?
BodyMap enables professionals and organizations to frame cognitive instability within a systemic regulatory context.
Across clinical, performance, or corporate settings, this supports:
• Earlier identification of regulatory stress patterns
• Integration of nutritional and recovery strategies
• Structured communication around cognitive fatigue
• Complementary positioning alongside psychological or performance programs
BodyMap supports cognitive resilience by reinforcing regulatory coherence rather than isolating single behavioral variables.
Explore how BodyMap can support your professional framework
Contact us to discuss integration within your clinical, performance, or preventive setting.
